| Climbing Areas | ||
Climbing FAQ | ||
| Articles | ||
Best of Rec.Climbing | ||
About Tradgirl | ||
by Dawn Alguard
I came home from the gym one night and found what I assumed was a chigger bite beneath the elastic of my sports bra. I'd heard about climbers getting chiggers at the Gunks. The bites--similar in appearance to a very large mosquito bite--are intensely itchy and appear in warm, moist, constricted areas. My bite hardly itched at all.
"These aren't so bad," I thought.
Over the next few days the bite increased in size, but it still didn't itch much. Then a red rash started to appear. Each day it grew larger. The entire area felt warm to the touch and looked kind of puffy. Finally, on day six, I made a doctor's appointment.
"Make sure you get tested for Lyme disease," a friend said.
I shrugged it off. I'd never seen a tick and the rash looked nothing like a bulls-eye; it was oblong and mottled with a ragged edge. The next morning I took a quick peek in the mirror. The rash had grown again and now I could see a vague bulls-eye pattern.
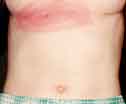 My rash didn't look anything like a bulls-eye until day 6 |
Luckily I was diagnosed early and completely cured. There's no reason to believe that my brief infection will ever bother me again. But not all Lyme disease stories have such happy endings. You can reduce your risk of infection and serious complications by asking yourself the following questions:
Am I at risk?
-
The greatest number of reported cases occur in the Northeastern, Middle Atlantic and upper Midwest states although Lyme disease has been found in almost every US state and in many other countries. The top 10 states for Lyme Disease, representing 90% of reported cases, are: New York, Connecticut, Pennsylvania, New Jersey, Wisconsin, Rhode Island, Maryland, Massachusetts, Minnesota and Delaware, but there's also a concentration of Lyme disease in northernwestern California.
You're most likely to get Lyme disease during the late spring or summer.
What can I do to avoid being bitten by a tick?
-
Unfortunately, many of the usual suggestions for preventing Lyme disease infection don't work very well for climbers. Avoiding wooded and grassy areas during the late spring and early summer months would certainly cut into your climbing, and it might be difficult to climb wearing long sleeves, long pants, and high rubber boots with your pants tucked into your socks.
You can, however, follow the recommendations to dress in light-colored clothes (makes ticks easier to spot before they attach themselves), to apply DEET to exposed areas*, and to check yourself thoroughly for ticks after possible exposure. Ticks start from the ground and climb upwards until they meet an obstruction. This makes any area with elastic suspect. Very small ticks may best be found by feel. Experts recommend a shower after exposure to rinse off any ticks that are not yet attached. As you wash, feel for small bumps.
* No, DEET won't harm your rope. See Blue Water's Dynamic Rope Care
Will I know if I've been bitten by a tick?
- Not necessarily since the bite itself is usually painless. Deer ticks are small to begin with and the juveniles, the ones that bite during climbing season, are about the size of a small freckle. The tick may remain attached for up to 48 hours but when it has finished feeding it will drop off by itself. You may never know it's there.
What if I find a tick?
-
The current recommendation for tick removal is to use a pair of fine-point tweezers to gently pull the tick's fangs away from your skin. Many of the recommendations for tick removal made in the past, such as burning off the tick with a cigarette end or smothering it in Vaseline, have now been determined to increase your chances of becoming infected.
Luckily, being bitten by a tick, even one that is carrying Lyme disease, does not guarantee that you will be infected.
How will I know if I have Lyme disease?
-
Approximately 80% of patients will get a rash at the site of the bite. The rash may resolve into the classic bulls-eye look--rings of red, broken by rings of white--but it may remain formless. It may develop anywhere from days to weeks after the initial bite. In dark-skinned people, the rash may look more like a bruise. The area may feel warm or tender and may itch.
Any rash (or bruise in darker-skinned people) that grows in size is a source of concern. A small rash at the site of the bite that doesn't grow is probably a localized reaction to the bite itself.
The rash may be accompanied by flu-like symptoms. Some people experience the flu-like symptoms without the rash or the rash without any other symptoms.
If you climb in a high-incidence area, you should keep an eye on any bug bite. If a rash develops around it, see a doctor to be tested. You should also consider seeing a doctor if you've been in a high-incidence area and develop flu symptoms without having been exposed to the flu.
What happens if I get Lyme disease?
- You'll be put on antibiotics. An initial course of 3 to 6 weeks is common. The prognosis varies considerably depending on how quickly the disease is caught and treated. If the disease is caught early, the initial course of antibiotics will probably be 100% effective.
What happens if I don't get treated?
-
The rash will disappear on its own eventually, perhaps in less than a week, along with any other symptoms you may have had. But in 3 to 5 months you may start to experience secondary symptoms. The most common secondary symptom is pain in the large joints. Other symptoms include chronic fatigue, neurological disorders, kidney disorders and heart disorders. If the disease isn't discovered until secondary symptoms start appearing, longer courses of antibiotics, intravenous antibiotics, and other courses of treatment may be necessary. Most cases of Lyme disease are eventually cured but some people suffer from lifelong complications.
If you have a suspect rash and for some reason you are not able (or not willing) to see a doctor immediately, consider taking a picture of your rash. Tests for Lyme disease aren't very reliable, so clinical evidence is important in making a diagnosis. If secondary symptoms later develop, a photo of the original rash will be helpful.
Is there a vaccine?
- There is currently one FDA approved vaccine called LYMErix. The vaccine consists of a series of three shots, spread over a year. The first shot should be administered in March. Maximum resistance to Lyme disease (approximately 80%) is not reached until after the third shot. It is not known at this time whether the vaccine continues to be maximally effective for more than a year after the last shot. Evidence appears to indicate that booster shots will be necessary. Also, LYMErix does not prevent the transmission of any tick-borne disease other than Lyme disease.
Should I get the vaccine?
-
The CDC recommends that people aged 15 to 70 who are at high risk should consider getting the vaccine. The vaccine is not recommended for people who are already suffering from Lyme arthritis or women who are pregnant.
However, there is considerable controversy over the vaccine, including pending lawsuits from people who claim that the vaccine caused Lyme disease in them. (The CDC, as of June 1999, does not agree that this is the case.) When you talk to your doctor, don't be surprised if he or she is less than enthusiastic about the vaccine. Many doctors, and most of the Lyme-related organizations, are taking a wait-and-see attitude about the vaccine.
Another vaccine, developed by Rx Technologies, Inc. is currently undergoing clinical trials. If this vaccine is approved, it promises a better solution. Rx Technologies' vaccine appears to provide lifelong immunity in a single dose and to protect against a wider spectrum of tick-borne diseases. But it may be years before the vaccine is FDA approved.
- Having Lyme disease once doesn't make you immune in the future. Fortunately, you can still consider the vaccine as long as you've been completely cured.
Where can I go for more information?
-
The Center for Disease Control's Lyme disease page
American Lyme Disease Foundation
Lyme Disease Network
The Lyme Disease Foundation
Lyme Alliance, Inc.